

I see patients every week as a dietitian in both corporate and clinical world , and I can tell you with certainty that PCOS is one of the most misunderstood conditions I encounter in my practice. Women arrive having already spent years trying to make sense of symptoms they could not explain irregular cycles, persistent acne, weight that would not shift no matter what they tried, facial hair they were quietly ashamed of. Many of them had been told their results were “normal.” Others had been handed a diagnosis without any real explanation of what it actually meant for how they should be living, eating, or thinking about their own bodies. Some even think it is spiritual.
What strikes me most is how rarely food enters the conversation in any specific or useful way. “Eat healthy” is said. Sometimes “lose weight.” But what does that actually look like for a Ghanaian woman sitting across from me at the clinic? What does it mean for someone who grew up eating banku and okro soup, who cooks with palm oil, who has never owned a food scale or measuring cups and does not intend to? What does it mean for a woman who is already tired, already frustrated, and has already tried cutting things out without results?
That is the gap I want to address here my dear women. Not general advice repackaged from a Western nutrition textbook. Not a list of superfoods she cannot find in her local market. But a clear, honest, explanation of why food matters in PCOS and how the foods already sitting in Ghanaian farms and kitchens may be some of the most powerful tools available. Let’s delve straight into why we are here.
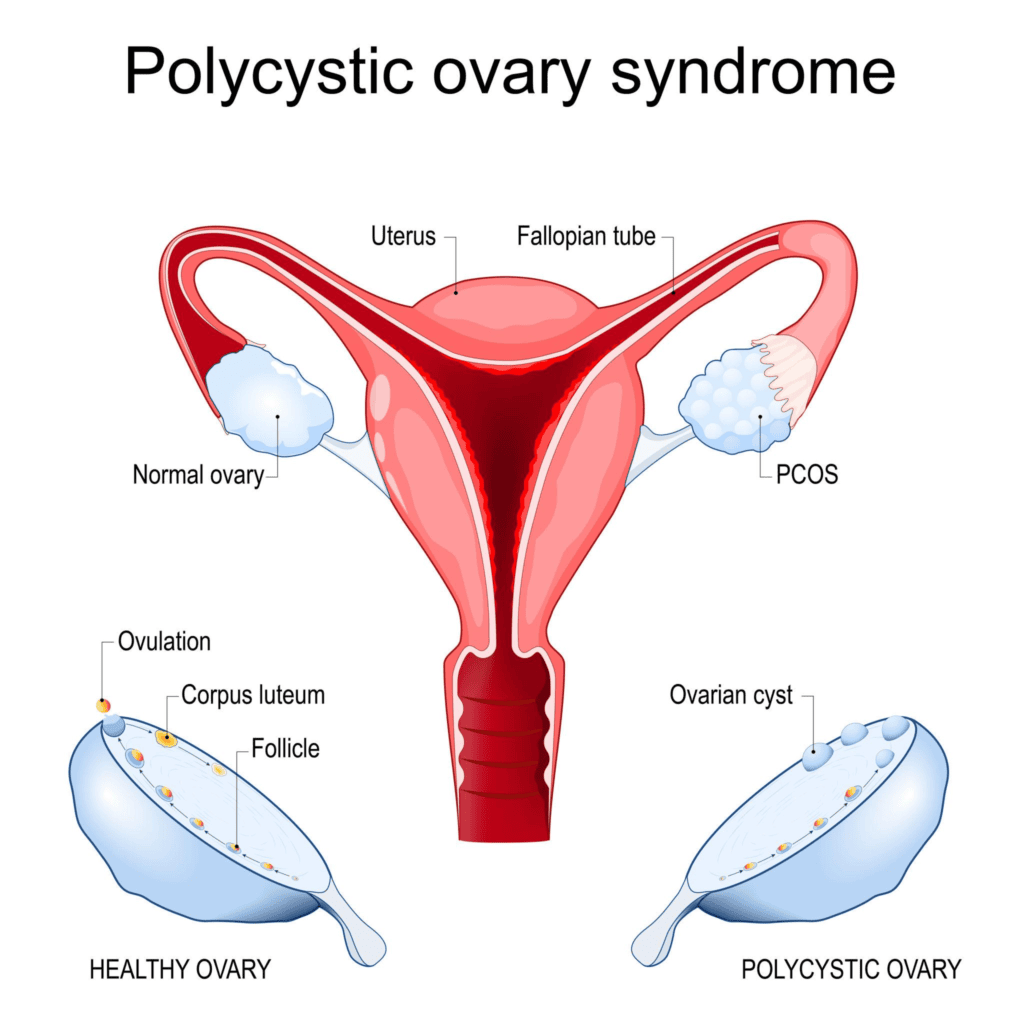
PCOS, or Polycystic Ovary Syndrome, is a hormonal condition that affects roughly one in ten women of reproductive age globally and research suggests the burden in West Africa may be comparable or higher, partly because of how frequently it goes undiagnosed (Teede et al., 2023). It causes irregular or absent periods, difficulty conceiving, persistent acne, unwanted facial or body hair, and weight that tends to accumulate around the abdomen. The name refers to the appearance of the ovaries on ultrasound small follicles that have not fully matured but PCOS is not primarily an ovarian disease. It is a whole-body metabolic and hormonal condition.
Many women in Ghana are living with PCOS without knowing it. Symptoms are frequently dismissed as stress, “the way your body is,” or simply irregular periods that “will sort themselves out.” The reality is that PCOS, left unmanaged, can affect long-term metabolic health, fertility, and emotional wellbeing. But it is also highly responsive to lifestyle and food in particular.
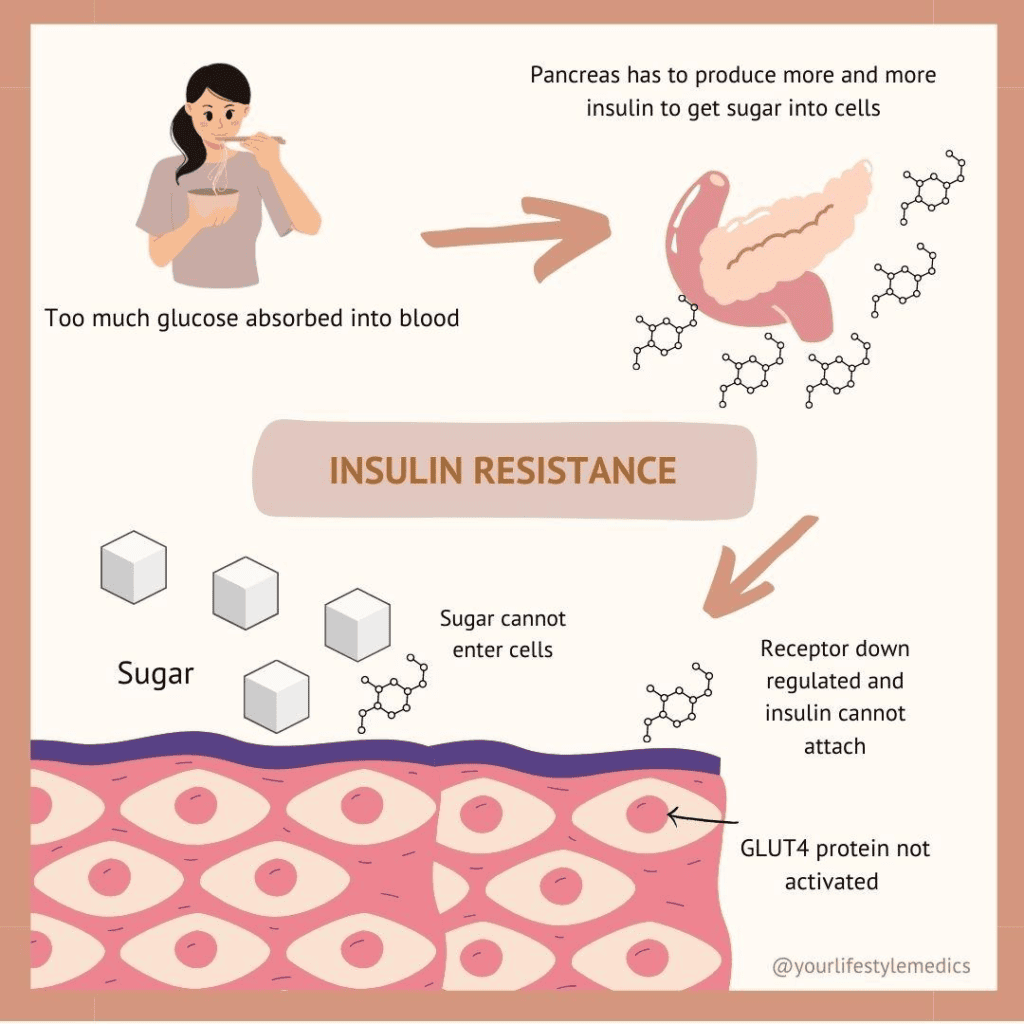
The key to understanding PCOS is insulin resistance a problem that affects majority of women with the condition, regardless of their weight (Moran et al., 2013). Insulin is the hormone that helps the body use sugar from food for energy. When cells stop responding to insulin properly, the pancreas compensates by producing more and more of it. The trouble is that high insulin levels signal the ovaries to produce excess male hormones, called Androgens. It is those androgens that drive the acne, the facial hair, and the menstrual irregularities that women find so distressing. The hormonal problem showing on the outside starts with how the body is handling food on the inside. I hope you are still here with me.
There is a second layer that makes this more complex. Most women with PCOS also carry a state of low-grade, chronic inflammation not the visible kind like a swollen wound, but a quiet background disruption in the immune system (Barrea et al., 2021). This inflammation makes insulin resistance worse. And insulin resistance feeds the inflammation. The two run in a loop. Processed foods, refined sugars, and heavily fried foods keep that loop turning. Foods rich in fibre, healthy fats, antioxidants, and polyphenols help break it.
What this means practically is that food is not just a side note in PCOS management. For many women, dietary change is the most direct and accessible lever they have for shifting what is happening hormonally often more immediately than medication alone.

Let me give you a practical story . My patient, let’s call her Akos, 31 years old, from the Oti Region came to me after being diagnosed with PCOS. She was eating the way many Ghanaian women eat: fufu with soup, banku with okra, rice and stew, occasional fish or chicken. She was not eating badly by any common standard. But she had been skipping breakfast in an attempt to lose weight, she sometimes fast the whole day and that single habit was doing significant harm.
When you skip breakfast, especially after a night of long fasting, your blood sugar drops and your stress hormone cortisol rises. The body reads this as a threat and produces more insulin when you eventually eat, trying to compensate. Over time, this pattern deepens insulin resistance and keeps androgen levels elevated. Guess what Akos body was caught in exactly this cycle.
We did not put her on a foreign diet. We did not ask her to buy anything unusual or count a single calorie. We simply restructured what she was already eating. We worked around what’s available to her. She started having breakfast every morning a typical example was oats meal with seeds, or a boiled egg with whole wheat bread and a piece of fruit on some days. She swapped processed breakfast to high fiber meals for breakfast. She made sure vegetables stews, salads or soup covered at least half her plate at main meals. She replaced her afternoon sweet drink with hibiscus juice made without added sugar. Her water intake improved as days went by, she started engaging in consistent physical activities 3-4 times a week. Don’t forget she was always checking in with her coach to monitor her progress, within three to six months of consistency, her fasting insulin had dropped measurably, her periods became more regular, her energy improved noticeably, and her skin began to clear. Everything she used came from her local market and discipline.

Unripe plantain is a standout example. Unlike ripe or fried plantain, it has a low glycaemic index releasing glucose slowly into the bloodstream and avoiding the insulin spikes that worsen PCOS symptoms. It is also rich in resistant starch, which feeds beneficial gut bacteria and supports the gut-hormone connection that researchers increasingly recognise as important in PCOS (Barrea et al., 2021).
Beans, cowpeas, and lentils deserve special attention. They provide slow-digesting carbohydrates, plant protein, and a compound called inositol specifically myo-inositol and D-chiro-inositol that has been shown in multiple clinical trials to improve insulin sensitivity, reduce androgen levels, and support more regular ovulation (Unfer et al., 2017; Nestler & Unfer, 2023). waakye or beans containing meals are genuinely therapeutic choices, backed by evidence.
Oily fish like mackerel, sardines, and tilapia provide omega-3 fatty acids, which reduce the chronic inflammation underlying PCOS and have been shown to lower testosterone levels in women with the condition (Kite et al., 2022). Leafy vegetables like kontomire, ayoyo, and alefu are rich in magnesium a mineral consistently found to be low in women with insulin resistance, and that plays a direct role in how insulin receptors function.
Oats are worth including specifically for their beta-glucan content a type of soluble fibre shown to improve insulin sensitivity and lower total cholesterol (Moran et al., 2013). Millet and sorghum, staples in northern Ghana, have a naturally lower glycaemic load than refined grains and are rich in B vitamins and minerals that support hormonal health. Fermented foods like kenkey and brukina support gut microbiome diversity, which emerging research connects to oestrogen metabolism and inflammatory regulation in PCOS (Barrea et al., 2021).

| Nutrient | Role in PCOS | Local Ghanaian Sources |
| Magnesium | Supports insulin signalling; frequently deficient in women with PCOS | Kontomire, alefu, groundnuts, pumpkin seeds |
| Omega-3 fatty acids | Reduces chronic inflammation; lowers androgen levels | Mackerel, sardines, herrings, tilapia |
| Vitamin D | Deficiency linked to insulin resistance and irregular cycles | Sunlight (daily), oily fish, egg yolks |
| Inositol (myo & D-chiro) | Improves insulin sensitivity, ovulation, and cycle regularity | Beans, cowpeas, oats, citrus fruits |
| Dietary fibre | Slows glucose absorption; feeds beneficial gut bacteria | Legumes, leafy greens, unripe plantain, oats, millet |
| Zinc | Supports androgen metabolism and skin health | Meat, shellfish, pumpkin seeds, legumes |
| Chromium | Enhances insulin receptor sensitivity | Whole grains, broccoli, meat, eggs |
| Iron | Often low in women with heavy PCOS-related periods | Red meat, liver, beans, leafy greens paired with vitamin C foods |

I want to be careful here, because I have seen too many women come to me already carrying guilt about food. I see the confusion on what to eat and what not to. The goal is never to create a list of forbidden foods or to make eating feel like punishment. But I want to be honest about what the evidence shows.
Sugary drinks are at the top of my concerns for women with PCOS. Malt drinks, bottled fruit juices, fizzy drinks, and some comertial sobolo made with large amounts of added sugar all push glucose into the bloodstream rapidly with nothing to slow it down driving up insulin in exactly the way PCOS does not need. In my clinical experience, addressing sugary drinks is one of the single most impactful changes a woman with PCOS can make.
Heavily refined carbohydrates white bread eaten daily, biscuits as regular snacks, large plates of white rice without adequate vegetables or protein sustain the insulin and inflammation cycle when they form the backbone of every meal. None of these foods need to be eliminated permanently. But eaten as the foundation of daily eating, they keep the cycle running. Skipping meals as a weight management strategy also backfires in PCOS, raising cortisol and worsening insulin resistance over time (Witchel et al., 2019).

Something I want to name, because it is real: living with PCOS takes a quiet emotional toll that clinical conversations rarely make space for. The acne that comes back. The weight that does not shift despite genuine effort. The period that does not arrive, or arrives unpredictably. The worry about fertility. The shame around body hair. These are not small things.
When I sit with a patient and she realises that her body has not been failing her it has been responding rationally to a hormonal environment she was not told about and did not cause something often shifts. She becomes a participant in her care, not a victim of her body. That shift matters enormously, and it is part of why I believe in taking the time to explain, not just prescribe.

I never begin with a rigid meal plan after thorough nutritional assessment, I start by asking what a woman normally eats, when she eats, and what her day actually looks like. But across most of my patients, a handful of consistent changes create the biggest early improvement:

Food cannot cure PCOS, and I want to be clear about that. Some women will also need medication for fertility, blood sugar management, or specific hormonal issues and there is no shame in that. But the evidence is consistent: the right nutritional approach, one that is specific, culturally grounded, and sustainable within someone’s real life, can meaningfully change how a woman with PCOS feels, how her hormones behave, and how much agency she has over her own body (Teede et al., 2023). The foods that support this are in our markets and our kitchens. They just need to be understood and used intentionally.
Barrea, L. et al. (2021). Dietary patterns and PCOS: A review with a focus on gut microbiota. Nutrients, 13(2), 584. https://doi.org/10.3390/nu13020584
Escobar-Morreale, H. F. (2018). Polycystic ovary syndrome: Definition, aetiology, diagnosis and treatment. Nature Reviews Endocrinology, 14(5), 270–284
Kite, C. et al. (2022). Exercise and nutrition interventions in women with PCOS: A systematic review. Nutrients, 14(18), 3756.
Moran, L. J. et al. (2013). Dietary composition in the treatment of PCOS: A systematic review. Journal of the Academy of Nutrition and Dietetics, 113(4), 520–545.
Nestler, J. E. & Unfer, V. (2023). Myo-inositol and D-chiro-inositol in PCOS. Frontiers in Endocrinology, 14, 1103862.
Teede, H. J. et al. (2023). Recommendations from the 2023 international evidence-based guideline for PCOS. Human Reproduction, 38(1), 3–9.
Unfer, V. et al. (2017). Myo-inositol effects in women with PCOS: A meta-analysis of randomized controlled trials. Endocrine Connections, 6(8), 647–658.
Witchel, S. F. et al. (2019). Polycystic ovary syndrome: Pathophysiology, presentation, and treatment. Journal of the Endocrine Society, 3(8), 1545–1573.

Join Weight Goals with Aba’s WhatsApp community and gain exclusive access to our hub of articles and recipes. Be part of a supportive community, receive valuable insights, and stay up-to-date with the latest in nutrition, fitness, lifestyle, and medicine. Elevate your weight goals journey by joining us today.

Nutrition consultation available online